Introduction
Maxillary anterior teeth are very important in achieving successful aesthetics. Several factors contribute to this success which includes patient’s healing capabilities, level and condition of existing soft and hard tissues and provisional and final restorations.
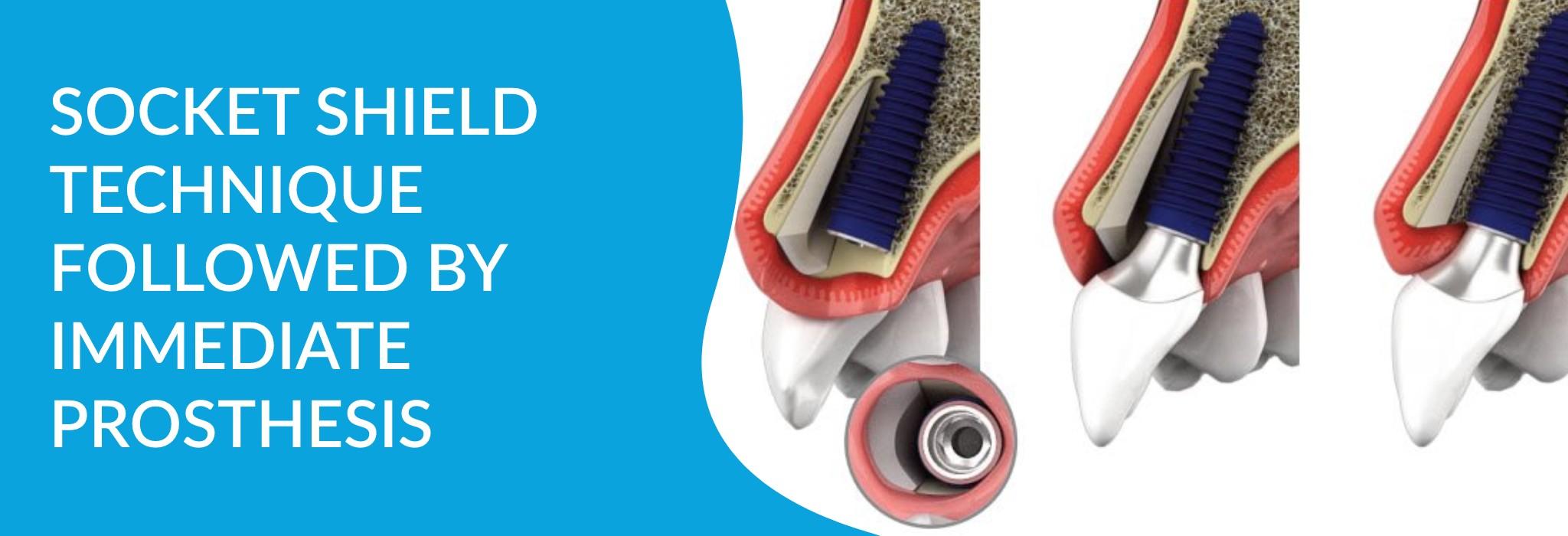
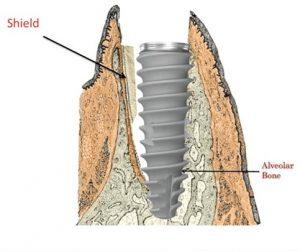
Tooth extraction is followed by severe bone alterations both in height and width. Such re-modelling can make implant placement a challenging task mainly due to deficient facial bone. However, it is possible to overcome this challenge by carrying out Socket Shield technique by partial extraction.
The following case outlines the technical basis of SST and demonstrates its importance in anterior implant planning.
Case Details
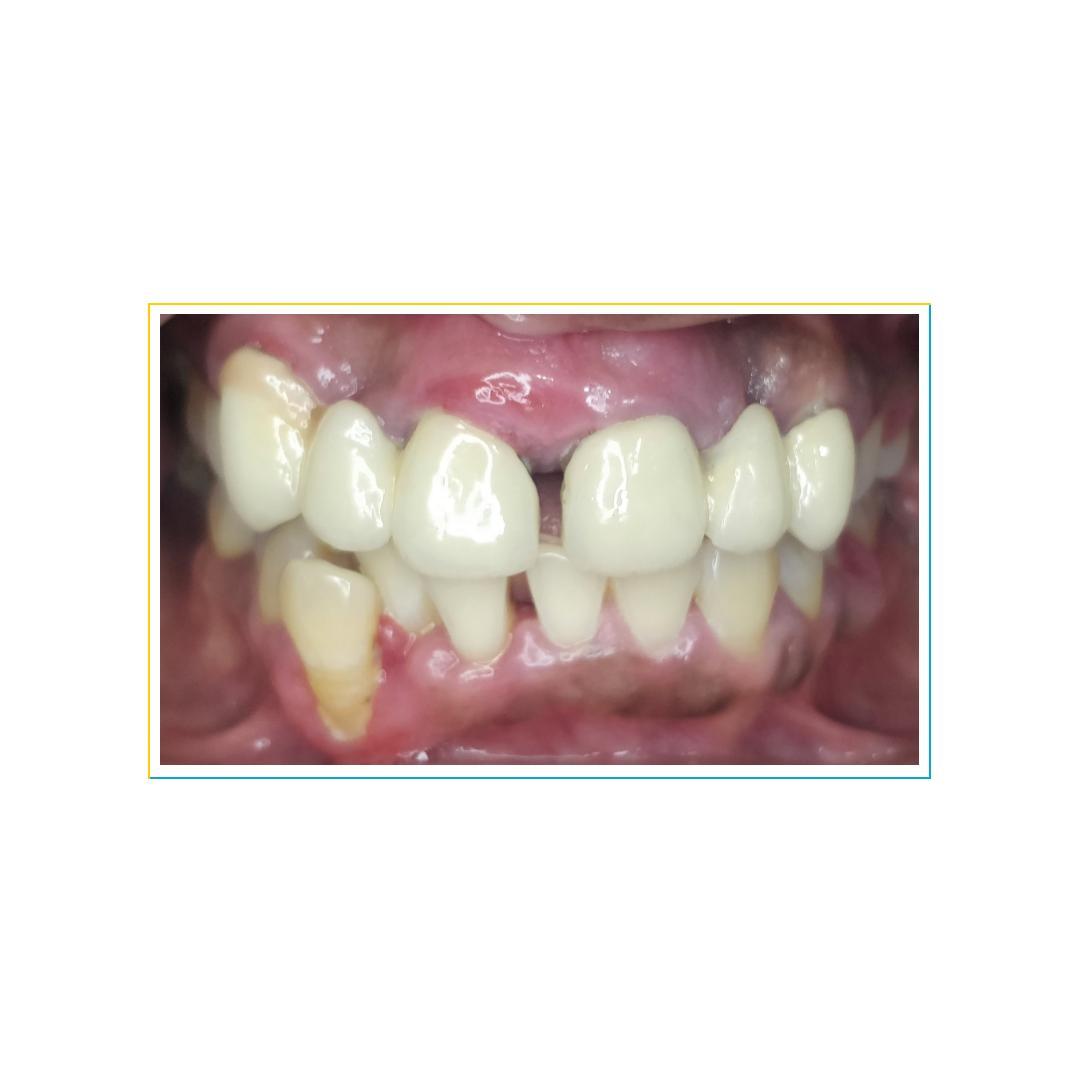
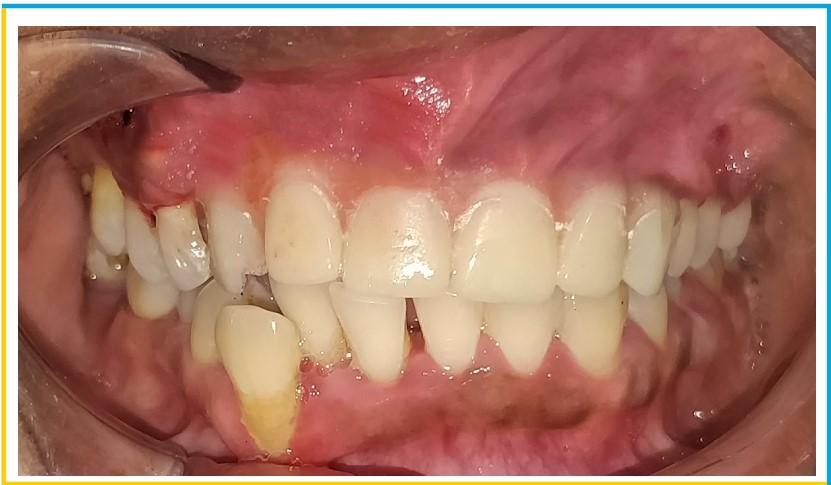
A 46 year old female patient with no medical history, presented with appalling aesthetics.The patient had high smile line and had a history of wearing fixed prosthesis wrt 11, 13 & 21, 23 with midline diastema since 8 years. Clinical examination showed bulky prosthesis with irregular and short margins and severe gingival inflammation.
On radiographic examination, the central incisors and prosthesis deemed hopeless, so removal of prosthesis along with 11, 21 was suggested . Also, thin buccal cortical bone was evident, so a socket shield technique by partial extraction of 13, 23 was planned.
Case Planning
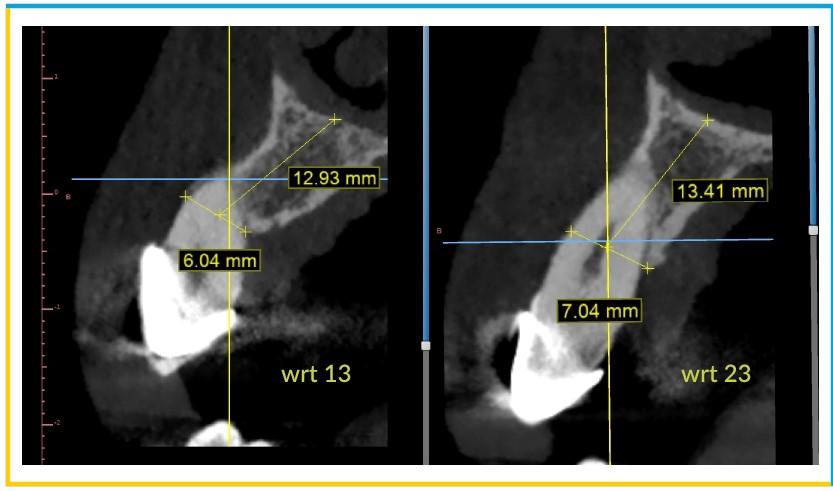
- Patient’s CT was obtained and the planning was done on Blue Sky Bio software. The anticipated site wrt 13 & 23 were viewed in Cross – sectional and Tangential windows . It was observed that there was a very thin buccal plate available wrt 13 &23.
- A measuring scale was used to define the measurements of the available bone. The length was measured from the crest of the bone to the nasal floor which was around 12mm and the crestal width was around 6 -7mm in the right canine region.
- On the left canine region, the length was around 14mm and the crestal width was around 7mm.
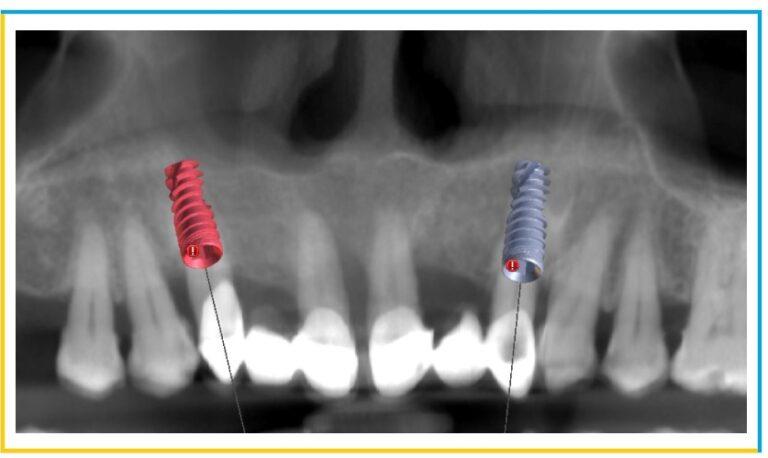
- The final dimensions of the Implants decided were: wrt 13 (4.2×11.5mm) & wrt 23 (4.2x13mm).
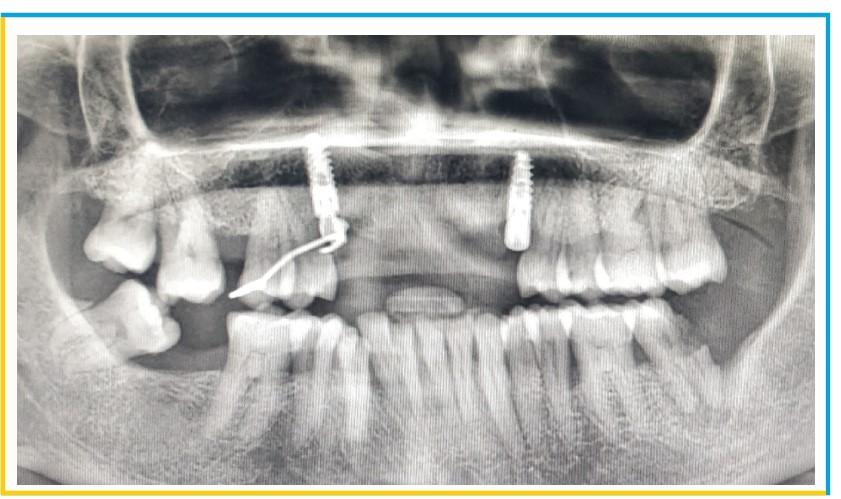
- The anticipated placement of the Implants in the desired sites were viewed in panoramic window.
Case Presentation
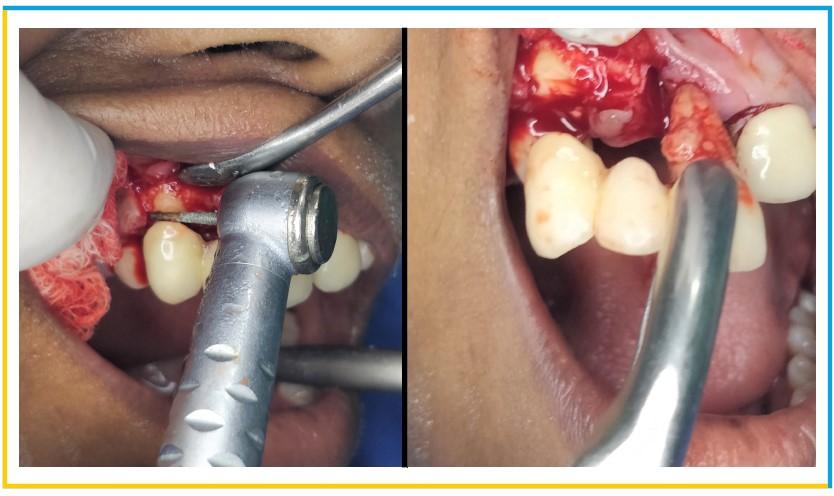
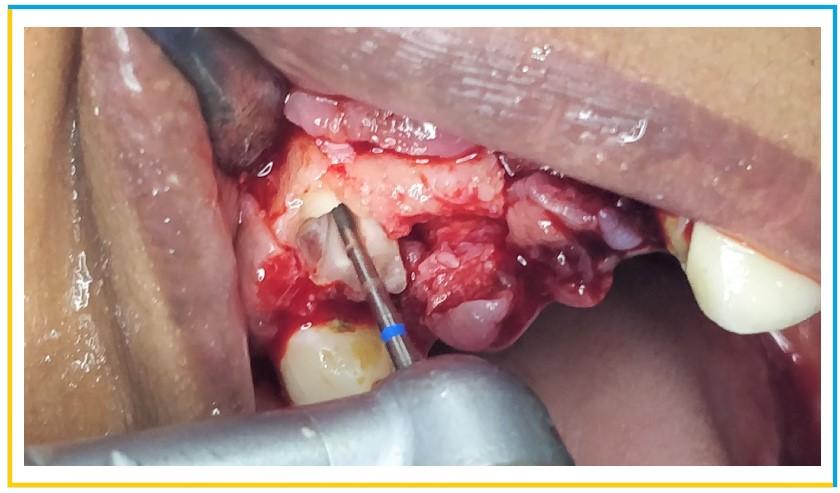
- Vertical and crevicular incisions were given to raise a full thickness flap and all the granulation tissue was removed. The tooth was sectioned bucco-palatally using PET (partial extraction theraphy) bur kit . This was intended to preserve the buccal 1/3rd of the root intact and undamaged. After thorough sectioning of the root, x-ray was taken to ensure the right path of the cutting.
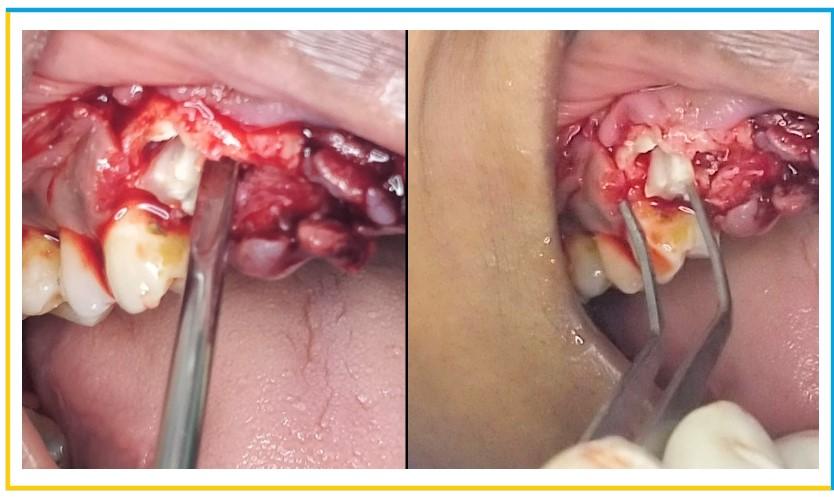
- The palatal section of root was then carefully removed without traumatizing the buccal root section using Periotome and root forceps. The remaining buccal half of the root section was then shaped properly and reduced to the level of the alveolar crest. Curettage was done of the extraction socket to remove any granulation tissue.
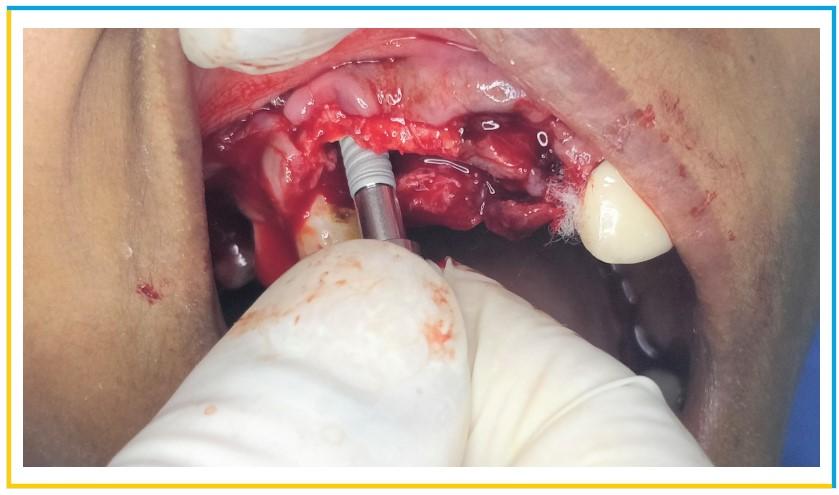
- Implant placement phase was initiated using a lance drill to engage the palatal aspect of the socket so that the buccal half of root would remain intact. A desired length of 11.5mm was achieved using the lance and pilot drill. Subsequent diameter drills were used to place the desired implant of diameter 4.2mm.
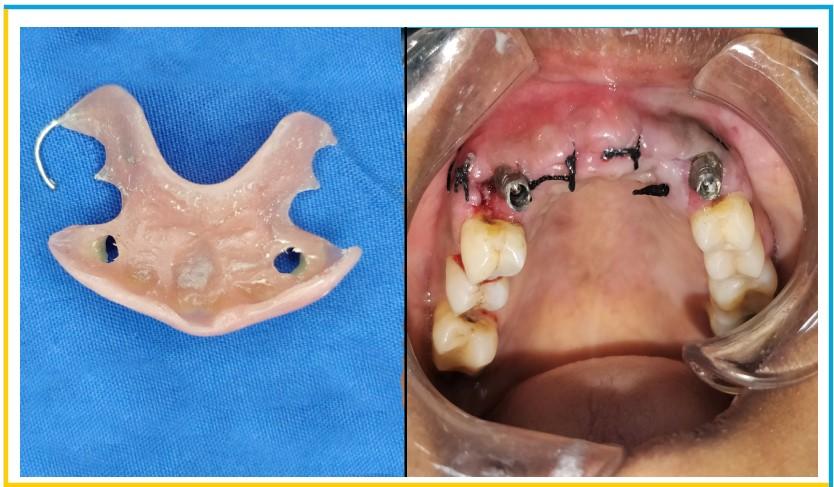
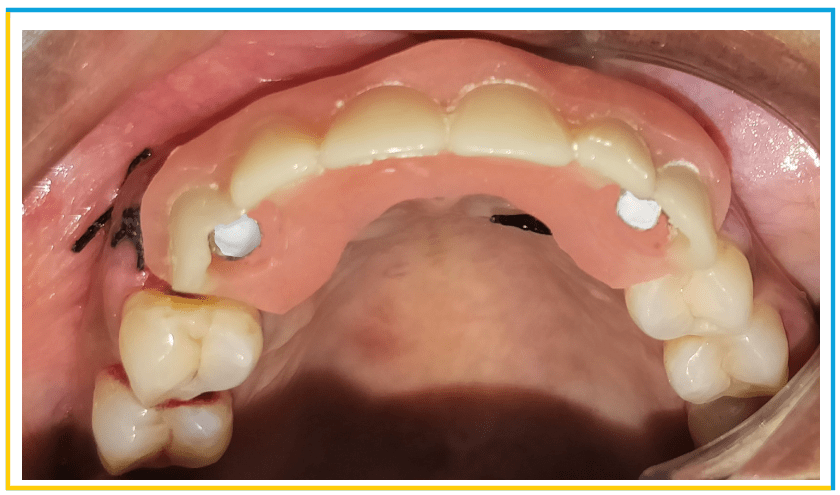
- After the implant placement, a screw-retained temporary prosthesis was fabricated, chairside as per routine protocol for immediate implant placement in the esthetic zone. For this, temporary cylinders were tightened on the MUAs and holes were drilled in the prefabricated RPD at the temporary cylinders site.
- Following fabrication of the interim restoration, a meticulous occlusal check was performed to ensure non-functional loading. Postsurgical instructions included antibiotics and analgesic medication and chlorhexidine 0.12% oral rinse. At 2 weeks, the patient was asked to return for a postoperative evaluation.